Effective pain management relies on detailed nursing care plans, often utilizing PDF resources for standardized protocols. These plans address complex needs,
considering age, cognition, and cultural factors for optimal patient outcomes.
Defining Pain and its Impact on Patients
Pain, a subjective experience, significantly impacts patients physically, emotionally, and functionally. Effective nursing care plans, often documented in PDF format, acknowledge this complexity. Unmanaged pain can lead to increased anxiety, depression, and decreased quality of life, hindering recovery and rehabilitation.
Stigma and bias, particularly affecting women’s pain assessment, necessitate a thorough and individualized approach. Comprehensive pain management, guided by evidence-based guidelines – frequently available as PDF resources – aims to alleviate suffering and restore optimal functioning. Understanding the multifaceted nature of pain is crucial for developing a patient-centered nursing care plan, ensuring holistic well-being.
The Importance of Comprehensive Pain Assessment
Comprehensive pain assessment is foundational to effective nursing care, often detailed within standardized PDF protocols. This involves gathering both subjective (patient’s description) and objective (physiological indicators) data. Accurate assessment guides appropriate interventions and prevents undertreatment, particularly in vulnerable populations like older adults.
Nursing journals focusing on pain management, accessible online, emphasize the need to address stigma and bias during assessment. Utilizing validated pain scales, documented within PDF guidelines, ensures consistent and reliable data collection. A thorough assessment informs the development of an individualized care plan, maximizing patient comfort and promoting optimal healing.

Components of a Nursing Care Plan for Pain
Detailed PDF nursing care plans include subjective and objective data, assessment tools, diagnoses, interventions, and evaluation criteria for effective pain management.
Subjective Data Collection: Patient’s Pain Experience
Gathering a patient’s subjective pain experience is crucial for a comprehensive nursing care plan, often guided by PDF templates. This involves detailed questioning about the pain’s location, intensity, quality (e.g., sharp, dull, aching), onset, duration, and aggravating/relieving factors.
Explore the patient’s perception of pain, its impact on daily life, and their coping mechanisms. Document their verbal and nonverbal cues, including facial expressions and body language. Utilize open-ended questions to encourage detailed descriptions. PDF resources often provide standardized questionnaires to aid this process, ensuring thoroughness and consistency in data collection, ultimately leading to personalized pain management strategies.
Objective Data Collection: Physiological Indicators of Pain
Objective data collection, often supported by PDF-based assessment guides, focuses on physiological signs indicating pain. Monitor vital signs – increased heart rate, blood pressure, and respiratory rate are common indicators. Observe for physical manifestations like pupil dilation, sweating, muscle tension, and guarding behaviors.
Assess the patient’s facial expressions and body posture for signs of discomfort. PDF protocols may include checklists for these observations. Document any changes in neurological function or activity levels. These objective findings, combined with subjective reports, create a complete picture, informing a targeted nursing care plan for effective pain management.
Pain Assessment Scales and Tools
Accurate pain assessment, often guided by PDF resources detailing various scales, is crucial for effective care planning. Utilize tools like the Numerical Rating Scale (NRS), asking patients to rate pain from 0-10. The Visual Analog Scale (VAS) employs a line for marking pain intensity.
For those with communication difficulties, the Faces Pain Scale – Revised (FPS-R) offers a visual representation. PDF guides often provide instructions for proper administration and interpretation. Consistent use of these tools, documented within the nursing care plan, ensures objective monitoring and facilitates tailored interventions.
Numerical Rating Scale (NRS)
The Numerical Rating Scale (NRS), frequently detailed in PDF nursing care plan guides, is a widely used pain assessment tool. Patients rate their pain intensity on a scale of 0 to 10, with 0 representing ‘no pain’ and 10 signifying ‘worst possible pain.’
PDF resources emphasize the importance of clear instructions and patient understanding. Regular NRS assessments, documented within the care plan, provide a quantifiable measure of pain levels. This allows nurses to track treatment effectiveness and adjust interventions accordingly. Consistent application ensures reliable data for informed clinical decision-making.
Visual Analog Scale (VAS)
The Visual Analog Scale (VAS), often included in PDF-based nursing care plans, presents a 10cm line representing a spectrum of pain intensity. Patients mark a point on the line corresponding to their perceived pain level, with anchors like “no pain” and “worst imaginable pain.”
PDF guides highlight the VAS’s simplicity and ease of use. Measurements are taken in millimeters, offering a more granular assessment than the NRS. Accurate documentation within the care plan is crucial for tracking changes. Nurses utilize VAS data to evaluate intervention effectiveness and tailor pain management strategies, ensuring patient comfort and well-being.
Faces Pain Scale – Revised (FPS-R)
The Faces Pain Scale – Revised (FPS-R), frequently found within PDF nursing care plan resources, utilizes a series of facial expressions to gauge pain intensity. It’s particularly valuable for patients with communication difficulties, including children and those with cognitive impairment.
PDF guides emphasize selecting the face that best represents the patient’s current pain. The scale ranges from “no hurt” to “worst pain possible.” Consistent application and documentation within the care plan are vital. Nurses leverage FPS-R data to understand patient experiences and adjust interventions, promoting effective pain relief and improved quality of life.

Nursing Diagnoses Related to Pain
PDF nursing care plans commonly utilize diagnoses like acute pain, chronic pain, and impaired comfort, guiding interventions for effective symptom management.
Acute Pain
Acute pain, frequently addressed in PDF-based nursing care plans, arises from a specific injury or illness with a predictable trajectory. These plans emphasize comprehensive assessment utilizing scales like NRS and VAS to quantify pain intensity. Interventions focus on pharmacological management – often opioid or non-opioid analgesics – alongside non-pharmacological approaches such as relaxation techniques and distraction therapy.
PDF resources detail administration guidelines, monitoring for adverse effects, and evaluating intervention effectiveness. Goals center on reducing pain to a tolerable level, improving functional ability, and promoting patient comfort. Documentation within the care plan meticulously tracks pain scores, interventions implemented, and patient responses, ensuring a data-driven approach to care.
Chronic Pain
Chronic pain nursing care plans, often available as PDF documents, differ significantly from acute pain management. These plans prioritize long-term strategies focusing on improving quality of life and functional capacity. PDF resources emphasize a multidisciplinary approach, integrating pharmacological interventions with physical therapy, psychological support, and complementary therapies.
Assessment includes exploring the impact of pain on daily living, coping mechanisms, and psychological well-being. Goals center on pain reduction, enhanced self-management skills, and minimizing disability. Careful monitoring for opioid tolerance and dependence is crucial, as detailed in PDF guidelines. Regular evaluation and plan adjustments are essential for sustained improvement.
Impaired Comfort
Impaired comfort, frequently addressed in PDF-based nursing care plans, extends beyond physical pain to encompass emotional and psychological distress. These plans prioritize holistic interventions to alleviate suffering and promote well-being. PDF resources often detail non-pharmacological approaches like relaxation techniques, distraction therapy, and therapeutic communication.
Assessment focuses on identifying contributing factors to discomfort, including anxiety, fear, and social isolation. Goals involve enhancing coping mechanisms, promoting restful sleep, and fostering a sense of control. Careful attention to environmental factors, such as noise and lighting, is crucial. Regular evaluation, guided by PDF protocols, ensures individualized care.

Interventions for Pain Management
PDF nursing care plans detail pharmacological (opioid/non-opioid) and non-pharmacological strategies—relaxation, distraction, heat/cold—to effectively manage patient pain and improve comfort.
Pharmacological Interventions
PDF-based nursing care plans meticulously outline pharmacological approaches to pain management, emphasizing safe and effective medication administration. Opioid analgesics, when indicated, require careful documentation of dosage, frequency, and potential side effects—respiratory depression, constipation, and nausea—demanding vigilant monitoring.
Non-opioid analgesics, such as acetaminophen and NSAIDs, are often utilized for mild to moderate pain, with attention to contraindications like renal impairment or bleeding risks. The care plan details appropriate pain reassessment intervals post-medication administration, ensuring therapeutic effectiveness.
Furthermore, these plans often incorporate adjunctive medications to manage breakthrough pain or address specific pain qualities. Adherence to hospital protocols, readily available in PDF format, is crucial for minimizing adverse events and optimizing patient comfort.
Opioid Administration Guidelines
PDF nursing care plans detail stringent opioid administration guidelines, prioritizing patient safety. Thorough pain assessment before administration is paramount, alongside a complete allergy history and review of concurrent medications. Careful dosage calculation, utilizing weight-based protocols, is essential, with a second nurse verification often required.
Monitoring for respiratory depression—assessing respiratory rate, oxygen saturation, and level of consciousness—is critical post-administration. Naloxone availability and staff competency in its use are documented within the plan.
Plans also address proactive management of common opioid side effects like constipation, utilizing bowel regimens. Comprehensive documentation of pain scores, medication effectiveness, and any adverse reactions is mandatory, aligning with hospital PDF protocols.
Non-Opioid Analgesic Use
PDF-based nursing care plans emphasize a multimodal approach to pain, prioritizing non-opioid analgesics when appropriate. Acetaminophen and NSAIDs are frequently included, with detailed guidelines regarding maximum daily dosages and contraindications—particularly regarding renal and hepatic function.
Plans outline the importance of assessing for gastrointestinal risks with NSAID use, often recommending prophylactic strategies. Adjuvant analgesics, like gabapentin or pregabalin for neuropathic pain, are addressed, specifying titration schedules and monitoring parameters.
Documentation within the PDF should reflect the patient’s response to these medications, alongside any observed side effects, ensuring a holistic and individualized pain management strategy.
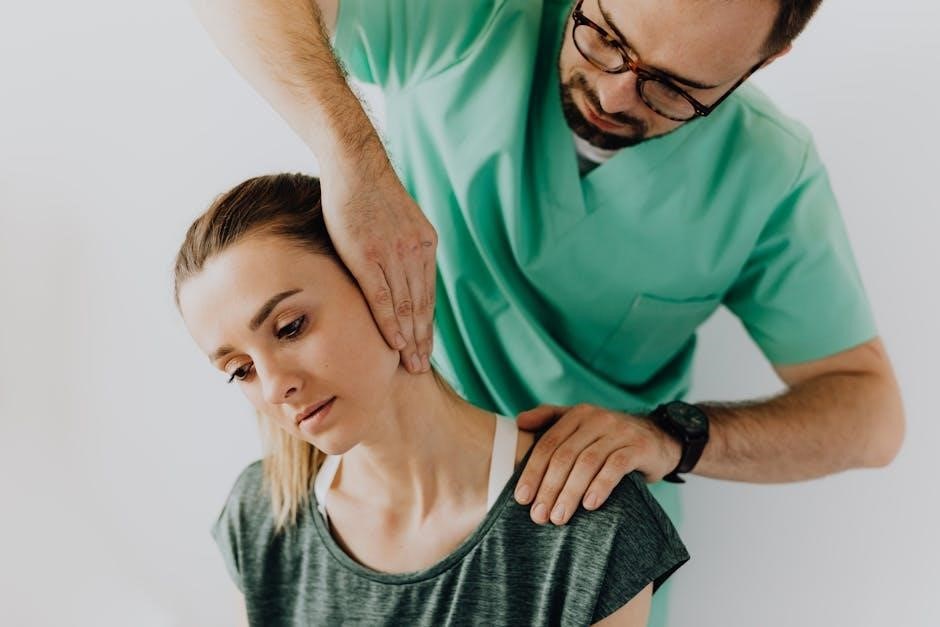
Non-Pharmacological Interventions
Nursing care plan PDFs highlight the crucial role of non-pharmacological techniques in complementing analgesic medications. Relaxation techniques, such as deep breathing and guided imagery, are detailed, including implementation steps and patient education materials.
Distraction therapy, utilizing music, television, or conversation, is outlined as a strategy for acute pain management. Heat and cold application protocols are included, specifying appropriate temperatures, durations, and safety precautions to prevent skin damage.
The PDF emphasizes individualized approaches, documenting patient preferences and evaluating the effectiveness of each intervention, fostering a holistic pain management plan.
Relaxation Techniques
Nursing care plan PDFs extensively detail relaxation techniques as vital non-pharmacological pain management strategies. Progressive muscle relaxation, involving systematic tensing and releasing muscle groups, is thoroughly explained with step-by-step instructions for nurses to guide patients.
Guided imagery scripts, designed to evoke peaceful and calming mental images, are often included as appendices within the PDF. Deep breathing exercises, focusing on diaphragmatic breathing, are presented with clear instructions and rationales for pain reduction.
The PDF stresses the importance of a quiet environment and patient education regarding the benefits and practice of these techniques.
Distraction Therapy
Nursing care plan PDFs highlight distraction therapy as a crucial non-pharmacological intervention for pain management, shifting the patient’s focus away from the painful stimulus. These resources detail various methods, including engaging activities like listening to music, watching videos, or playing games.
PDF documents often suggest age-appropriate distractions; for example, storytelling for children or puzzles for adults. Virtual reality applications, offering immersive and engaging experiences, are increasingly recommended and described within these plans.
The PDF emphasizes the importance of patient preference and tailoring distractions to individual interests for maximum effectiveness, alongside consistent assessment of pain levels.
Heat and Cold Application
Nursing care plan PDFs extensively cover heat and cold therapy as accessible, non-pharmacological pain management techniques. These documents detail specific protocols, including application duration, temperature guidelines, and skin protection measures to prevent injury.
PDF resources clarify when to utilize heat – for chronic muscle tension and stiffness – versus cold – for acute injuries and inflammation. They emphasize the importance of patient assessment, contraindications (like impaired sensation), and careful monitoring of skin integrity.
Detailed instructions within the PDFs guide nurses on proper application techniques, ensuring patient safety and maximizing therapeutic benefits, alongside consistent pain level evaluations.

Evaluation of Pain Management Effectiveness
Nursing care plan PDFs stress ongoing assessment using pain scales, observing patient responses, and adjusting interventions for optimal pain control and comfort.
Monitoring Patient Response to Interventions
Utilizing a nursing care plan, often accessed as a PDF, requires diligent monitoring of the patient’s response to implemented interventions. This includes frequent reassessments using the chosen pain scale – NRS, VAS, or FPS-R – documenting both pain intensity and characteristics.
Observe for non-verbal cues indicating pain, such as facial expressions, body language, and vital sign changes. Evaluate the effectiveness of pharmacological interventions, noting any adverse effects.
Assess the impact of non-pharmacological techniques like relaxation or distraction. Consistent documentation within the care plan PDF is crucial for tracking progress and informing adjustments to the plan, ensuring individualized and effective pain management.
Adjusting the Care Plan Based on Evaluation
Regular evaluation of the nursing care plan, often a PDF document, dictates necessary adjustments. If pain remains uncontrolled despite interventions, reassess the initial assessment for inaccuracies or overlooked factors.
Consider escalating pharmacological interventions, consulting with the physician regarding dosage or alternative analgesics. If non-pharmacological methods prove ineffective, explore additional techniques or tailor existing ones to the patient’s preferences.
Document all changes within the PDF care plan, justifying the rationale behind each modification. A dynamic, patient-centered approach, guided by ongoing evaluation, is essential for optimizing pain management outcomes and ensuring comfort.

Special Considerations in Pain Management
PDF-based care plans must address unique needs of older adults, those with cognitive impairments, and cultural differences impacting pain perception and expression.
Pain Management in Older Adults
Geriatric patients often present unique challenges in pain management, necessitating specialized PDF-guided nursing care plans. Age-related physiological changes, such as decreased renal and hepatic function, impact drug metabolism and excretion, requiring lower dosages and careful monitoring. Comorbidities are prevalent, potentially interacting with analgesics.
Cognitive impairment can hinder accurate pain reporting, demanding observational assessments and proxy reporting. Fear of addiction and side effects may lead to underreporting. Non-pharmacological approaches, detailed in PDF resources, like relaxation and heat/cold therapy, become crucial adjuncts. Comprehensive PDF protocols should emphasize a holistic approach, considering functional status and quality of life alongside pain control.
Addressing Pain in Patients with Cognitive Impairment
Patients with cognitive impairment struggle to articulate pain, demanding innovative PDF-based nursing care plans. Reliance on behavioral indicators – facial expressions, vocalization, body language – is crucial, detailed within specialized PDF guidelines. Observational pain assessment tools, like the PAINAD scale, become essential.
Caregivers’ input is vital, documented within the PDF care plan, as they recognize subtle changes. Pharmacological interventions require cautious titration, starting with low doses to minimize side effects. Non-pharmacological methods – music therapy, gentle touch – are often well-tolerated and detailed in PDF resources. A consistent, individualized approach, guided by a comprehensive PDF, is paramount for effective pain relief.
Cultural Considerations in Pain Assessment and Treatment
Cultural beliefs profoundly influence pain expression and coping mechanisms, necessitating culturally sensitive PDF-based nursing care plans. Some cultures encourage stoicism, while others permit overt displays of pain; PDF protocols must acknowledge this. Communication styles vary – directness, use of interpreters – impacting accurate assessment, detailed in PDF guides.

Treatment preferences also differ; some may favor traditional remedies alongside conventional medicine, documented within the PDF. Avoid stereotyping; individualize care based on the patient’s specific beliefs, outlined in the PDF. Respectful inquiry about cultural practices is essential. A culturally tailored PDF care plan enhances trust and improves pain management outcomes.

Resources for Nursing Care Plan Development (PDF Focus)
Numerous online databases offer PDF nursing care plan templates, while hospital PDF protocols standardize pain management, ensuring consistent, evidence-based practice.
Online Databases for Nursing Care Plans
Several reputable online databases provide readily accessible nursing care plans, often available as downloadable PDF documents. These resources streamline the planning process, offering pre-written plans for various pain conditions, including acute and chronic pain scenarios. RegisteredNurseRN.com and NursesLab.com are frequently cited examples, offering comprehensive plans adaptable to individual patient needs.
However, it’s crucial to remember that these plans should serve as a starting point, not a replacement for individualized assessment and clinical judgment. Always verify the information against current evidence-based guidelines and hospital protocols. Utilizing PDF versions allows for easy printing and integration into patient charts, promoting efficient documentation and care coordination. Remember to critically evaluate the source and tailor the plan to the specific patient presentation.
Utilizing Hospital-Specific Pain Management Protocols (PDF)
Hospitals frequently maintain detailed, PDF-formatted pain management protocols to ensure standardized, evidence-based care. These documents outline specific assessment procedures, pharmacological and non-pharmacological interventions, and escalation pathways for uncontrolled pain. Accessing and adhering to these protocols is paramount for legal and ethical practice.
Familiarize yourself with your institution’s specific guidelines, often found on the intranet or through the nursing resource center. These PDFs typically include order sets, pain assessment tools, and algorithms for opioid and non-opioid administration. Utilizing these resources promotes consistency, reduces errors, and supports collaborative care. Always prioritize hospital protocols over generic online templates, ensuring patient safety and compliance with institutional standards.

